Classic studies from the Knobil laboratory have shown that GnRH releases from the infundibulum nucleus occur once per hour. Through the portal system of the pituitary gland, GnRH enters gonadotropic cells and stimulates the secretion of LH and FSH (also once an hour). This secretion can be reproduced in monkeys by pulsed administration of GnRH. A decrease in the frequency of impulse secretion of GnRH to 1 time per 3 hours (as occurs with hypothalamic dysfunction) leads to a decrease in the secretion of gonadotropic hormones.
About the reasons
Such ailments can be triggered by a variety of injuries that are directly related to physical injury to such a gland; the following examples can be given here:
- eating behavior is disordered (bulimia or its reverse anorexia may occur here);
- a person eats incorrectly;
- the head was susceptible to injury;
- there was exposure;
- genetic disorders;
- surgical intervention;
- other types of influences that can cause a pathological condition of such an organ.
If the hypothalamus is susceptible to damage, then a disruption in the process of hormonal production, which is necessary for the normal functioning of the human endocrine system, can be provoked. Quite a few hormones produced by the hypothalamus affect the pituitary gland, and its inflammation can cause irreversible consequences. So it is clear why diseases of the hypothalamus affect pituitary activity; here the close connection with the pituitary gland is obvious, and this already affects the condition of the adrenal glands, genital organs and thyroid gland.
It should be noted that severe hypothalamic dysfunction often occurs for reasons that doctors cannot accurately identify, since the pathology has not yet been fully studied. This may negatively affect the outcome of treatment.
What is the hormonal axis, arc
In the body there is a hierarchy (order of primacy) of endocrine organs. This means that there is a “commander” - the hypothalamus, its “subordinate” - the pituitary gland, and at the end of this axis there is an “ordinary performer” - the testicles. This interaction is called vertical, that is, orders from the hypothalamus of the brain reach the gonads in a descending manner.
The regulation of the work of these organs is not limited to the direct flow of commands. Testicular hormones can change the functions of the hypothalamus and pituitary gland in a feedback manner. This means that when there is a lack of sex steroids, the brain makes efforts to synthesize them. When there is an excess of male hormones, the hypothalamus inhibits the functioning of the glands. That is, the hypothalamic-pituitary-testicular axis is bilateral.
It should be noted that it is most correct to combine these organs into a single complex and consider them as an inextricable system. The terms hormonal "axis" or "arc" are introduced to describe the reactions that occur to make them easier to understand. They are most often used by bodybuilders to explain the effects of anabolic steroids.
We recommend reading the article about hypogonadism in men. From it you will learn about what hypogonadism is, the reasons for its occurrence in men, why it occurs in boys, age-related hypogonadism in men with diabetes, as well as the types and symptoms of the pathology.
And here is more information about endocrine infertility.
What are the symptoms?
If there are disturbances in the hypothalamus, then serious disruptions begin in the regulation of important functions in the human body:
- water and sodium balance are disturbed;
- unstable body temperature;
- unstable emotional state;
- poor sleep;
- height to weight ratio;
- blood pressure;
- lactation process in women.
As already noted, the pituitary gland is closely connected with the hypothalamus, so when the hypothalamus is disrupted, the pituitary gland is no longer able to function normally, and its reaction speed is impaired. Since the transmission of signals to the pituitary gland becomes untimely, this can cause a lack of certain hormones, which negatively affects the functioning of many organs and tissues in the human body. There may be a delay in puberty, impaired potency and libido, slower body growth, unstable weight, and impaired blood pressure.
What kind of organ is this
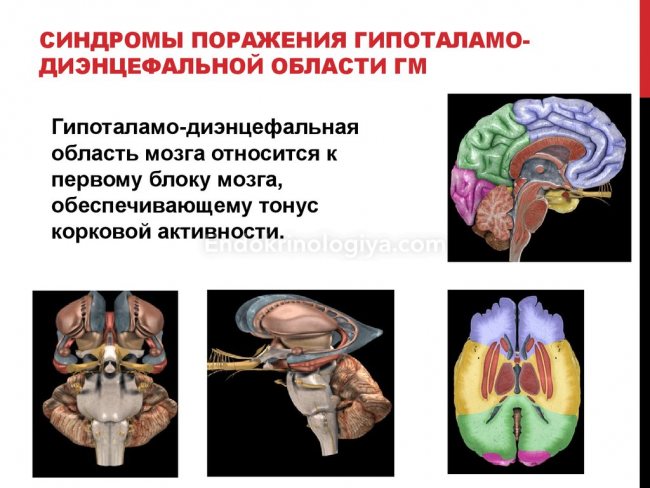
The diencephalon section influences the stability of the internal environment, ensures the interaction and optimal combination of individual systems with the holistic functioning of the body. An important structure produces a complex of hormones of three subclasses.
Neurosecretory and nerve conduction cells are the basis of an important element of the diencephalon. Organic pathologies in combination with damage to functions disrupt the periodicity of many processes in the body.
The hypothalamus has extensive connections with other brain structures and continuously interacts with the cerebral cortex and subcortex, which ensures an optimal psycho-emotional state. Decortication provokes the development of the “imaginary rage” syndrome.
Infection, tumor process, congenital anomalies, injuries to an important part of the brain negatively affect neurohumoral regulation, interfere with the transmission of impulses from the heart, lungs, digestive organs, and other elements of the body. Destruction of various lobes of the hypothalamus disrupts sleep, metabolic processes, provokes the development of epilepsy, diabetes insipidus, obesity, decreased temperature, and emotional disorders.
Not everyone knows where the hypothalamus is located. The diencephalon element is located under the hypothalamic sulcus, below the thalamus. The cellular groups of the structure smoothly transform into a transparent septum. The structure of the small organ is complex; it is formed from 32 pairs of hypothalamic nuclei, consisting of nerve cells.
The hypothalamus consists of three regions, with no clear boundary between them. The branches of the arterial circle ensure a complete supply of blood to an important part of the brain. A specific feature of the vessels of this element is the ability of protein molecules, even large ones, to penetrate through the walls.
Find out about the normal blood glucose level in women by age, the causes and symptoms of abnormal readings.
Adenoma of the left adrenal gland in men: what is it and how to get rid of the formation? Read the answer in this article.
Neurogenic diabetes insipidus
This disease most often develops because antidiuretic hormone is produced in insufficient quantities, all of which results in symptoms such as a constant feeling of thirst and frequent urination. If urination is prolonged, it can cause dehydration of the human body. As a result, a person constantly feels weak, gets tired quickly, becomes irritable, eats poorly, libido and potency are impaired, and there may be amenorrhea.
Tertiary hypothyroidism
The hypothalamic-pituitary system includes the thyroid gland, which is an auxiliary organ. There is a hormone called thyrotropin, it is a releasing hormone, it is produced by the hypothalamus, which, if necessary, gives a signal to the pituitary gland to produce such a hormone. It is he who is able to stimulate the thyroid gland so that it begins to produce hormones such as T3 and T4.
- the secondary form of the disease develops when the secretion of thyroid-stimulating hormone is impaired;
- the tertiary form is evidence of thyrotropin-releasing hormone deficiency or its suppression.
Those hormones that are produced by the thyroid gland are responsible for metabolic activity. If they are produced in insufficient quantities, metabolic activity becomes suppressed. And this is already accompanied by the following signs:
- a person’s weight is growing rapidly;
- memory, intelligence and speech decrease;
- blood pressure decreases;
- the heart rhythm is disrupted;
- the gastrointestinal tract works with disturbances;
- women may have infertility;
- the person becomes irritable;
- there is pain in the heart.
Of course, such signs do not 100% indicate the presence of just such a pathology.
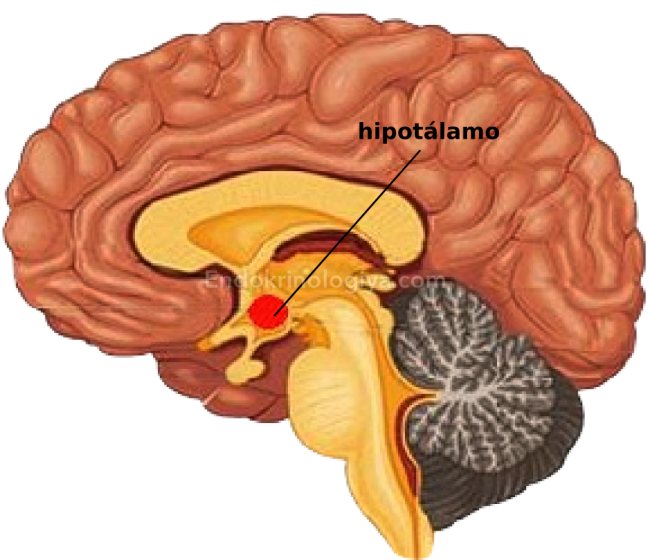
Hypothalamus
The central link for the pituitary-dependent glands is the hypothalamus. There is a close structural and functional connection between the hypothalamus and the pituitary gland, which made it possible to combine them into a single system - the hypothalamic-pituitary system.
The hypothalamus occupies the basal part of the diencephalon and borders the third ventricle. The hypothalamus contains numerous nerve cells, including neurosecretory cells, which are grouped into numerous nuclei. Currently, 32 nuclei have been described in the hypothalamus. The hypothalamus is conventionally divided into 3 sections: anterior, middle (mediobasal) and posterior. In the anterior part of the hypothalamus there are two largest (magnocellular) nuclei: the supraoptic (SO) and the paraventricular (PVN). These nuclei consist of large multipolar neurons containing large clumps of tigroid substance and characterized by a very high level of metabolic processes. Numerous secretory granules are always present in the cytoplasm of these cells. The supraoptic and paraventricular nuclei produce neurohormones. The supraoptic nucleus produces vasopressin (antidiuretic hormone), and the paraventricular nucleus secretes oxytocin. The axons of the nerve cells of the large cell nuclei of the hypothalamus are directed to the posterior lobe of the pituitary gland, where they end in thickenings on the surface of the blood capillaries. In these thickenings, neurohormones (Herring's bodies) accumulate, arriving here along the axons of neurosecretory cells. However, the axons of some cells of the supraoptic and paraventricular nuclei secrete their hormones into the capillaries of the median eminence, i.e. to the portal system. The activity of these cells is regulated by neurotransmitters that are produced at synapses lying on the surface of endocrine neurons. In addition, according to modern concepts, the hormones of these nuclei can be released into the blood through the posterior lobe of the pituitary gland, into the portal vessels and cerebrospinal fluid through the 3rd ventricle.
Vasopressin has a pronounced vasoconstrictor effect. In addition, it increases blood pressure, participates in the regulation of water metabolism, in particular, it enhances the processes of water reabsorption in the kidney tubules, which leads to a decrease in diuresis. Insufficiency of this hormone causes the development of diabetes insipidus or diabetes insipidus. Diabetes insipidus can be congenital or acquired. This disease is based on damage to neurosecretory cells that produce vasopressin, or disruption of the transport of this hormone to sites of secretion (for example, damage to the neurohypophyseal pathway).
Oxytocin is close in chemical composition to vasopressin, but specifically stimulates the contractility of the myometrium during childbirth. In addition, oxytocin causes contraction of myoepithelial cells present in the ducts of the mammary glands. When breastfeeding, numerous receptors in the peripapillary area are irritated. Nerve impulses enter the brain and then the hypothalamus, which leads to the activation of neurosecretory cells to produce oxytocin, which enters the mammary glands through the bloodstream and causes contraction of the myoepithelial cells, which causes milk to be squeezed into the baby’s mouth. The function of oxytocin in the male body has not been established.
In the anterior part of the hypothalamus there is a suprachiasmatic nucleus, which regulates human sexual behavior and circadian (circadian) rhythms (sleep and wakefulness, eating and rest, and others), that is, this nucleus is a kind of pacemaker for eating and drinking behavior.
In the middle part of the hypothalamus there are many nuclei, the most important of which are the parvocellular nuclei: arcuate and ventromedial. The neurosecretory cells of these nuclei are characterized by a high level of development of the triad of organelles, the presence of secretory granules, and a high level of metabolic processes. Short axons of neurons of small cell nuclei are directed to the median eminence (thickening of the ependyma of the 3rd ventricle), where they end on the surface of the capillaries into which neurohormones are released. These nuclei produce numerous hormones that have a stimulating effect on the endocrine cells of the anterior pituitary gland. These hormones are called “adenohypophystropic hormones”, “releasing hormones”, or “liberins”. In addition, hormones are produced here that have an inhibitory effect on the activity of endocrine cells of the anterior pituitary gland (these are statins). It is believed that each cell of the anterior pituitary gland produces its own liberin and its own statin. The predominance of one or the other determines the activation or inhibition of secretory activity of cells.
Thus, the hypothalamus determines the regulation of the secretory activity of the adenohypophysis. In addition, the hypothalamus is the center of the autonomic nervous system. In general, the hypothalamus can be considered a highly specialized structure that links the central nervous system and the endocrine system. It is like a complex switchboard that converts nerve signals into endocrine ones.
Pituitary
The pituitary gland is the king of the endocrine systems, as it has a regulatory influence on many organs and systems. The human pituitary gland consists of the anterior, tuberal, intermediate and posterior lobes. The mass of the pituitary gland is only 500 mg, and its dimensions are 1.5 x 1.0 cm. The pituitary gland develops from several sources. The development of the pituitary gland begins at the 4th week of embryogenesis. Initially, an epithelial cord grows from the roof of the oral cavity towards the brain - the pituitary pouch (Rathke's pouch). At the same time, a protrusion in the form of a funnel (pituitary funnel) appears from the interstitial medulla (bottom of the 3rd ventricle). The epithelium of the pituitary recess is a thin two-row layer, the height of which increases significantly by 6-7 weeks. At the same time, the epithelium of the anterior wall of the pouch has great histioblastic capabilities and in the 7-8 week embryo begins to actively proliferate into the surrounding mesenchyme in the form of strands of epithelial tubes. The growing cords determine the shape of the anterior lobe of the pituitary gland, forming its peripheral part. The central zone at this time remains filled with mesenchyme and is preserved as the site of the developing vascular system of the pituitary gland. Ultimately, as a result of strong proliferation of the epithelium of the anterior wall of Rathke's pouch, the anterior lobe of the pituitary gland is formed.
Increased proliferation of the epithelium of the posterior wall of the pituitary recess leads to the formation of the intermediate lobe of the pituitary gland, which in humans does not reach a high degree of development. Due to the fact that the anterior and intermediate lobes of the pituitary gland have a single epithelial origin and produce hormones, together they constitute the adenohypophysis (glandular pituitary gland).
As a result of the proliferation of neuroglia around the pituitary infundibulum, the posterior lobe of the pituitary gland is formed, which does not produce its own hormones. Due to its origin, the posterior lobe is called the neurohypophysis.
Thus, the pituitary gland consists of two embryologically, structurally and functionally different and independent parts: the adenohypophysis and the neurohypophysis.
The adenohypophysis includes the anterior lobe, a narrow intermediate lobe and a poorly developed tuberal lobe.
The pituitary gland is covered with a thin connective tissue capsule. The stroma is represented by very thin layers of loose, unformed connective tissue with a large number of reticulin fibers.
The anterior lobe of the pituitary gland is characterized by an abundant blood supply, which is represented by the vessels of the branches of the internal corotid artery. Due to this, the anterior lobe of the pituitary gland on a fresh section has a bright color. The anterior lobe accounts for about 75% of the mass of the pituitary gland. The anterior lobe consists of secretory cells - adenocytes, which are closely adjacent to each other and form cords or trabeculae that anastomose with each other. Between these cords there are numerous sinusoidal capillaries. Adenocytes have different sizes and shapes (from oval to polygonal). In relation to dyes, all adenocytes are divided into two groups: chromophobic (weakly accepting dyes) and chromophilic (well accepting dyes).
Chromophobe cells are called chief cells, as they make up 55-60% of all cells of the adenohypophysis. They are located in the middle of the trabeculae, have small sizes and light cytoplasm. Their organelles are poorly developed. According to modern concepts, chromophobe adenocytes include chromophilic cells after secretion and poorly differentiated cambial cells, which are the source of the formation of chromophilic cells.
Chromophilic cells are cells that accept dye well. They account for 45-50% of the total number of adenocytes. Chromophilic cells are divided into acidophilic (oxyphilic) and basophilic.
Acidophilic adenocytes are contained in an amount of 30-35%. These cells are round or oval in shape, medium in size, and their nucleus lies in the center. The cytoplasm of these cells contains numerous organelles, including the granular endoplasmic reticulum and the Golgi apparatus, which indicates the intensity of seritor processes.
Among acidophilic cells, two types of cells are distinguished: somatotropocytes and lacticotropocytes.
Somatotropocytes constitute the predominant cell type (40-65% of all cells of the adenohypophysis). These cells are small in size, but larger than chromophobe cells, round or even branched in shape. The core lies in the center or somewhat eccentrically. The cytoplasm contains numerous large granules, which can be located either evenly or at the periphery. The endoplasmic reticulum and mitochondria are poorly developed. However, in these cells there are many free ribosomes and the Golgi apparatus is well developed. Somatotropocytes produce somatotropic hormone (growth hormone). This hormone regulates growth and proportional development. The target organs for this hormone are bones, as well as formations rich in connective tissue (muscles, tendons, ligaments, internal organs). Stimulation of growth is carried out due to the anabolic effect of somatotropic hormone (increased transport of amino acids into the cell, acceleration of the processes of biosynthesis of protein and nucleic acids). At the same time, reactions associated with protein breakdown are inhibited.
In addition, growth hormone has a lipolytic effect, which leads to an increase in free fatty acids in plasma and their inclusion in energy metabolism. This helps preserve glucose and amino acids.
Somatotropic hormone stimulates the activity of osteoblasts and promotes intensive formation of the protein matrix of the bone. At the same time, the processes of mineralization of bone tissue intensify, resulting in calcium and phosphorus retention in the body.
This hormone activates macrophages, affects tissue differentiation, cell proliferation, and stimulates the proliferation of cartilage cells of the epiphyseal growth plate.
At the same time, scientists drew attention to the fact that when a somatropic hormone is introduced into an isolated cell culture, a noticeable increase in the growth of the latter is not observed. In this regard, the assumption arose that the stimulation of growth processes observed in the conditions of the whole organism is not the result of the direct action of this hormone. Most likely, under the influence of somatotropic hormone, the formation of certain intermediaries occurs, the influence of which leads to an anabolic effect. Such intermediaries are called somatomedins, which are proteins synthesized in the liver under the influence of growth hormone.
The secretion of somatotropic hormone is regulated by somatoliberin and somatostatin.
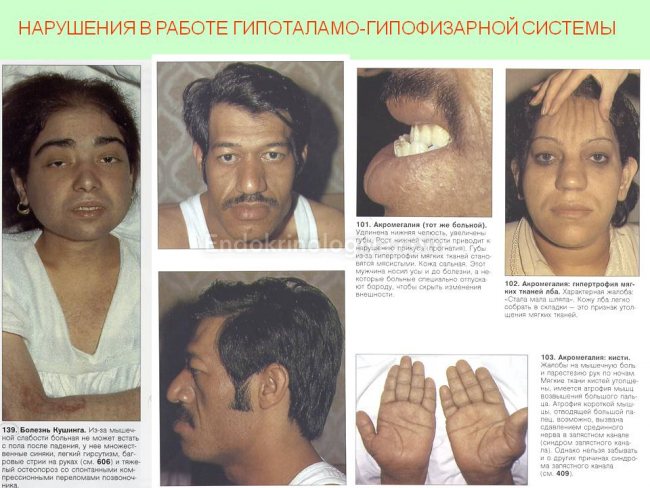
Insufficient formation of somatotropic hormone causes growth retardation in the child. Dwarfism associated with weakened pituitary function is called pituitary dwarfism and is characterized by short stature, delayed sexual development and satisfactory mental development. Excessive intake of this hormone in childhood causes gigantism. In adulthood, excess growth hormone leads to an increase in exposed parts of the body - acromegaly.
Lacticotropocytes constitute a less common population of cells (they account for only 1-2% of cells) of the adenohypophysis. These cells are larger than somatotropocytes. Organelles are better developed than in somatotropocytes, especially a lot of granular endoplasmic reticulum, mitochondria, ribosomes, and Golgi apparatus structures. There are few secretory granules in the cytoplasm. Until the onset of puberty in females, these cells are in an inactive state. During lactation, the number of organelles in them increases. Lacticotropocytes produce lacticotropic hormone (prolactin), which regulates the development of mammary glands (strengthens proliferative processes in them) and their secretion of milk. In addition, prolactin stimulates the formation of the corpus luteum. The male body contains very few lacticotropocytes. The role of lacticotropic hormone in the male body has not been established. It is believed to have an effect on prostate development.
The production of lactotropic hormone is regulated by prolactostatin and prolactoliberin.
The share of basophilic adenocytes accounts for only 4-10%. This is the largest population of cells in the anterior pituitary gland. These cells are irregular in shape with clear contours, with an eccentrically located nucleus. Their cytoplasm contains large granules that are stained with basic dyes. Among basophils, several types of cells are distinguished: thyrotropocytes, corticotropocytes and ganadotropocytes.
Thyrotropocytes are polygonal or branched in shape and lie near the capillaries throughout the substance of the anterior pituitary gland. Their share accounts for only 1.8-2.9%. The secretory granules are small and lie predominantly near the plasmalemma. The core is large, round, and lies eccentrically. Organelles are less developed than in other cells. Thyrotropocytes produce thyroid-stimulating hormone, under the influence of which the formation of iodine-containing hormones in the thyroid gland is stimulated by enhancing plastic processes in thyrotropocytes (protein synthesis, nucleic acids) and increasing oxygen absorption, which stimulates almost all stages of the synthesis of thyroid hormones. Thyroid-stimulating hormone also increases the activity of proteases that break down thyroglobulin.
Corticotropocytes also have an irregular or processed shape with long processes. These cells are distributed unevenly. Secretory granules lie near the plasmalemma. The organelles are moderately developed. These cells produce adrenocorticotropic hormone, which stimulates the growth of the zona fasciculata and zona reticularis of the adrenal cortex. The main effect of this hormone is expressed in its stimulating effect on the formation of glucocorticoids in the zona fasciculata of the adrenal cortex. Its influence on the glomerular and reticular zones is less pronounced. ACTH accelerates steroidogenesis and enhances plastic processes (protein biosynthesis, nucleic acids). In addition, this hormone has a lipolytic effect. Has an anabolic effect, enhances pigmentation. The production of this hormone is regulated by corticoliberin in the hypothalamus.
Gonadotropocytes are classified as basophils. Among them, there are two types of cells that produce two hormones: follicle-stimulating and luteinizing hormones. FSH-producing gonadotropocytes account for 2.2-3.5% and are more common in females than in males. These are large cells, round in shape, located mainly on the periphery of the adenohypophysis. The degree of development of organelles is determined by the level of the functional state of the cells. LH-producing gonadotropocytes are oval or polygonal in shape, there are fewer FSH-producing cells, and their granules are also somewhat smaller than those of the previous cells.
Follicle-stimulating hormone causes follicles to mature and prepare them for ovulation. Luteinizing hormone causes ovulation and stimulates the formation of the corpus luteum and the production of progesterone in it. In addition, luteinizing hormone stimulates the activity of Leydig cells to produce testosterone, and follicle-stimulating hormone stimulates spermatogenesis. The secretion of gonadotropins is regulated by hypothalamic gonadoliberin. The negative feedback mechanism is also significant: the secretion of both hormones is inhibited with an increase in the content of estrogen and progesterone in the blood, and the production of luteinizing hormone decreases with an increase in testosterone production.
With insufficient production of gonadotropic hormones of the pituitary gland, a delay in puberty is observed.
Morphology of the secretory process
All active types of cells of the adenohypophysis produce their secretion in the form of granules. The protein secretion is produced by the granular endoplasmic reticulum and is transported through its tubules to the structures of the Golgi apparatus, where the secretory product is condensed and formed into granules. In actively functioning cells, the Golgi apparatus is always hypertrophied. The hormone is released in various ways:
1. The granules undergo dissolution in the cell itself and vacuoles are formed.
2. The granules are completely pushed out of the cell into the intercellular space.
3. The granules approach the plasma membrane and undergo fragmentation and dissolution.
The tuberal lobe consists of strands of epithelial cells, between which are located the pituitary portal veins, connecting the primary capillary network of the median eminence and the secondary capillary network of the anterior pituitary gland. Among the epithelial cells there are single basophilic adenocytes.
The intermediate lobe of the pituitary gland in humans is very poorly developed. It accounts for only about 2% of the organ's mass. It is built from strands of multilayered epithelium, which contains chromophobe and basophilic adenocytes. Sometimes between the epithelial cells there are follicles resembling those in the thyroid gland.
In 1916, Smith and Allen observed discoloration of the skin of tadpoles after hypophysectomy. Three years later, Atwell, placing tadpoles in a crude extract of the pituitary gland, discovered a darkening of their skin. Only in 1938, Tsondek discovered that the darkening of the skin of amphibians was caused by an extract of the intermediate lobe of the pituitary gland. It has now been established that melanocyte-stimulating hormone (intermedin) is produced in the intermediate lobe, which enhances the formation of melanin (inducing the synthesis of tyrosinase) and, thereby, affects skin pigmentation, enhances visual acuity, and adaptation of the retina in the dark. In addition, this hormone stimulates the activity of the sebaceous glands and the production of pheromones. It is believed that lipotropic hormone is produced here, which stimulates fat metabolism.
The posterior lobe of the pituitary gland includes numerous nerve fibers , which are the axons of the neurosecretory cells of the hypothalamus (supraoptic and paraventricular), which together form the hypothalamic-pituitary tract, consisting of more than 100,000 unmyelinated nerve fibers. The terminal extensions of neurosecretory axons on the surface of capillaries contain neurosecretory granules and mitochondria of various shapes and sizes. The largest of the axon extensions are called Herring's bodies, where neurohormones are deposited. The posterior lobe contains numerous fenestrated capillaries. In addition, there are modified glial cells - pituicytes, which are branched or spindle-shaped and often contain pigment inclusions. Their nucleus is dense, and the organelles, including the granular and agranular endoplasmic reticulum, are poorly developed. Pituicytes are assigned a stromal function. The neurohypophysis does not produce its own hormones.
Thus, the pituitary gland is in close neurohumoral connection with the hypothalamus, forming the hypothalamic-pituitary system.
What types of developmental disorders can there be?
If growth hormone is produced in insufficient quantities, then a lack of gonadotropin may occur, and this is already fraught with the following serious disorders:
- puberty may not begin at all or may begin but not be completed;
- sexual development is premature;
- human growth slows down;
- body weight is growing rapidly;
- there is not enough T4 hormone, which can lead to hypothyroidism;
- sex hormones can have a negative effect.
If we talk about lesions of the hypothalamus in a focal form, they arise due to various types of trauma, tumor formations, or the development of inflammatory processes. All of them occur against the background of pronounced disturbances in the regulation of the vegetative type of internal organs. If the functioning of the hypothalamic-pituitary system is seriously disrupted, then there may be diencephalic syndromes, and such disorders are difficult to fight (with such a syndrome, irreversible changes can affect the brain), as well as with a violation of the pituitary function.
How is the pituitary gland connected to the hypothalamus and testes?
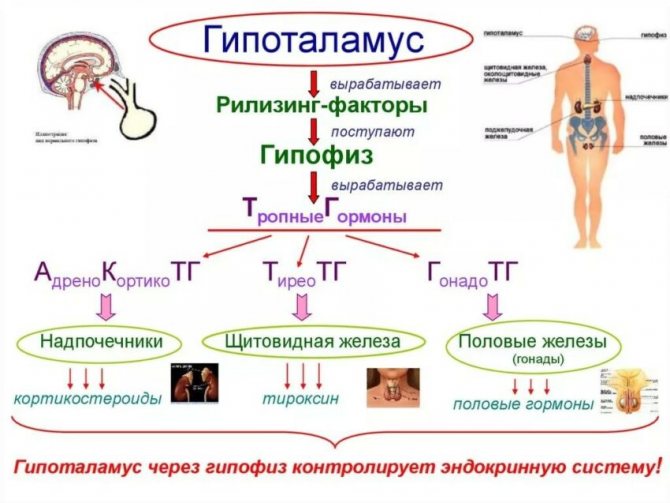
The hypothalamus produces gonadotropin releasing factor, or GnRH. If these terms are translated literally, they mean “gonadotropin-releasing.” When it enters the pituitary gland, the release of gonadotropic hormones begins. They are so named because they affect the gonads - the sex glands (testes in men).
The hypothalamus is the highest level of the endocrine system. His blood supply is structured in such a way that large protein molecules can penetrate through the barrier between the vessels and the brain. This organ analyzes the content of hormones, neurotransmitters, and trace elements in the blood. In this case, the concentration of testosterone, estradiol and inhibin B is important for the functioning of the hypothalamic-pituitary-testicular arc. All of them inhibit the production of gonadotropin.
The production of releasing factor for the reproductive system occurs in the form of rhythmic releases into the pituitary gland. If you introduce its analogue or stimulant into the body in a large dose, this will stop the release of GnRH.
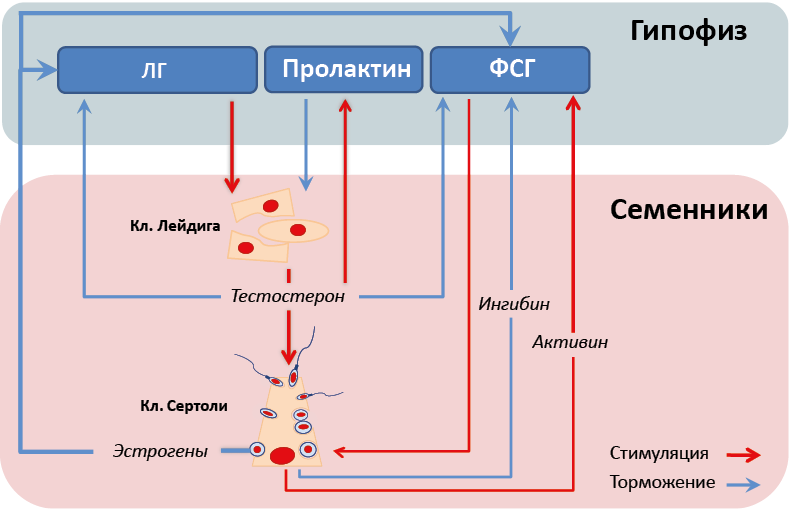
The pituitary gonadotropins include luteinizing hormone (LH) and follicle-stimulating hormone (FSH). They, in turn, ensure the formation of sperm and testosterone by the testicles. The first is primarily responsible for hormonal activity, and the second for cellular synthesis.
Testosterone is converted into estrogens using aromatase (an enzyme). Female hormones in men have the ability to suppress lutropin along with testosterone. There is even evidence that estrogenic influences are stronger, as well as inhibition of the synthesis of luteinizing hormone, causing both too high and low levels of blood estradiol.
Diagnostic methods
Diagnosis of ailments should be based on specific signs of associated diseases:
- blood tests are necessary, and first of all it is necessary to find out the hormonal level of the body;
- the brain must be followed by computed tomography and magnetic resonance imaging;
- It is imperative to examine organs that may be targets to identify potential problems that are not directly related to hypothalamic disease.
Diseases of different hypothalamus can sometimes disguise themselves as other diseases, since the symptoms are quite common in other diseases, so before making a diagnosis, you need to conduct thorough research using several methods. Only a specialist can determine the disease
Suppression of the hormonal axis
The concentration of testosterone in the blood can be negatively affected by the following factors:
- diseases of the brain, gonads due to infections, injuries, operations, tumors, vascular, autoimmune (with the formation of antibodies to one’s cells) diseases;
- congenital malformations of any of the organs: pituitary gland, hypothalamus, testicles;
- metabolic disorders (most often obesity, diabetes mellitus);
- age-related decrease in hormonal activity of the testicles;
- the use of medications that inhibit hormonal activity or excessively stimulate it.
With any of the options for suppressing the axis, symptoms manifest themselves in the form of a decrease in testosterone levels in the blood:
- general and sexual weakness, impotence;
- low level of sexual desire;
- mood swings, tendency to depression, irritability;
- weakening of intellectual control of behavior;
- decreased motility and sperm count;
- destruction of bone tissue;
- testicular atrophy (become smaller).
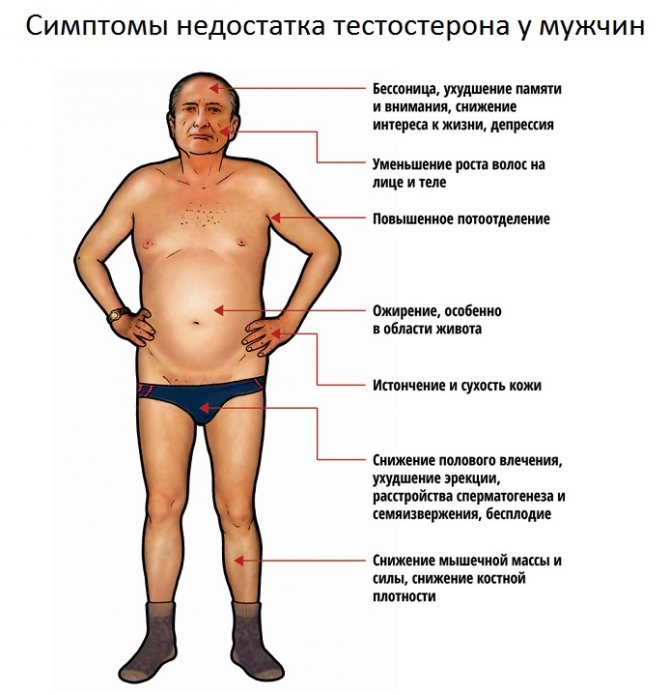
Exactly the same manifestations of androgen deficiency occur with the use of anabolic steroids. Since they are consumed at normal (baseline) testosterone levels, suppression of the hormonal axis occurs.
The hypothalamus reacts to excess steroids in the blood and inhibits the production of GnRH. As a result:
- the production of luteinizing hormone by the pituitary gland decreases;
- the concentration of sex steroid binding globulin increases;
- production of adrenocorticotropin and adrenal cortisol increases;
- the level of prolactin and estrogen increases, which further suppress all sexual functions;
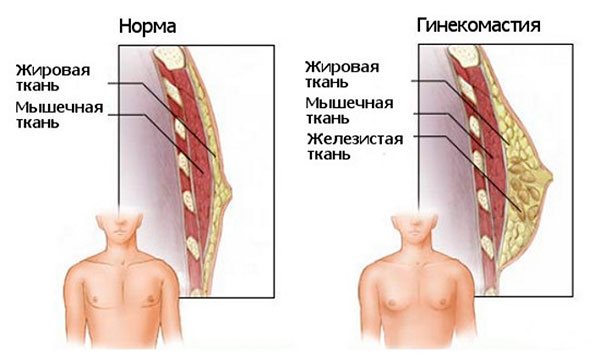
- the mammary glands become larger in volume, milk may be released from the nipples;
- Acne appears on the skin, swelling is noted.
If hormonal therapy is used against the background of a disease or age-related decline of the body, then androgens have the opposite effect:
- increase strength and endurance;
- stimulate sexual desire;
- improve the functioning of the heart and blood vessels;
- strengthen bone tissue;
- remove excess fat from the body;
- restore carbohydrate metabolism, stimulate glucose absorption.
Watch the video about the hypothalamic-pituitary-testicular arc:
But even in this case, any abuse of drugs, long-term use or increased dosages can be dangerous.
Maybe:
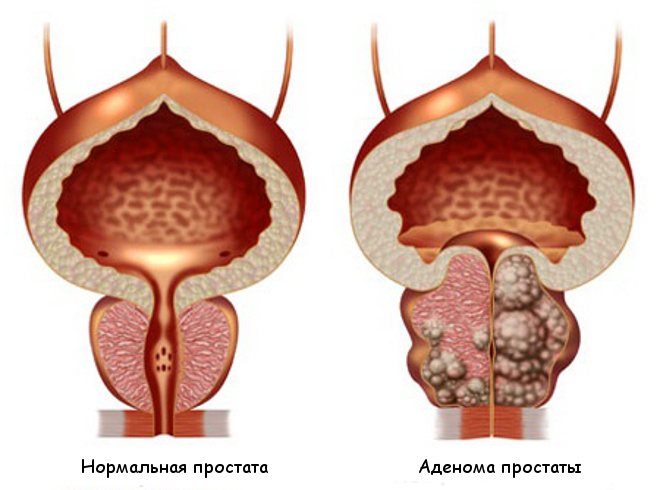
- increase in prostate volume;
- formation of an adenoma or cancerous tumor in the prostate gland;
- stopping breathing during sleep (night apnea syndrome).
How is treatment carried out?
As for treatment, everything is based on the cause of the specific nature of hypothalamic dysfunction. If a tumor-like formation acts as a catalyst for pathology, then it is necessary to use radiation therapy; if it does not have the desired positive effect or the dysfunction of the organ is in an advanced form, then surgery is indicated.
If the pathology is based on hormonal deficiency, then one of the most common treatment options is hormone replacement therapy. However, it often happens that the cause of dysfunction remains unknown; in such cases, symptomatic treatment is indicated. Very often, in order to cure such a pathology, medications are used that are used to treat non-sugar diabetes.
Disruption of the hypothalamus is treated individually; if we are talking about women in a state of pregnancy, then only medications are used, and if we are talking about men with underdeveloped genitals, then other means will be effective. The choice of treatment always remains with the attending physician, who is based on various factors. A folk remedy may be recommended, but it can only be treated as an additional option, but not the main one, replacing traditional treatment.
Restoration of the hypothalamic arch, pituitary gland and testes
Potential harm from anabolic steroids exists with any regimen of administration. Different people react to hormones to different degrees. This is due to the function of the liver, kidneys, lifestyle, and training intensity. With long-term use, side effects occur in almost all previously healthy people.
The problem of arch restoration is complicated by the fact that anabolic steroids and drugs to treat the consequences are not prescribed by doctors and without blood tests.
Rehabilitation of sexual function can be carried out by an andrologist or an endocrinologist. Several directions are recommended to normalize hormonal levels.
Physical activity
Based on studies of testosterone levels, signs of training that help its formation have been identified:
- medium pace and intensity;
- inclusion of all muscle groups, joints;
- about 10 repetitions, 4 sets and a pause before the next set of exercises for at least 1.5 minutes;
- total duration - about an hour;
- avoid overwork;
- limit or completely eliminate aerobic exercise (running, swimming), and give preference to strength training.
Watch the video about a set of exercises to increase testosterone:
Diet
Particular attention should be paid to protein intake from lean meat products, fermented milk drinks, and fish. Its level should be about 2-2.5 g per 1 kg of weight.
Healthy fats are found in avocados, nuts and peanut butter, and egg yolks. It is not recommended to eat more than a tablespoon of these products at one meal, since excess fat leads to a decrease in testosterone levels by almost a quarter, and it takes at least 8 hours to restore it.

To reduce the formation of female hormones, you should choose foods high in indole-3-carbinol. It is most abundant in broccoli, arugula, cauliflower and kohlrabi. The best option for consumption is short steaming or in the form of salads from fresh vegetables.
The diet must include:
- sufficient amount of fluid (dehydration disrupts fat and carbohydrate metabolism);
- products with zinc (participates in hormonal synthesis) - meat, pumpkin seeds, liver;
- vitamin D (inhibits the transition of the hormone to estrogens) - yogurt, oatmeal, fatty fish;
- magnesium (increases the proportion of active testosterone) – legumes, nuts and seeds, quinoa.

Lifestyle
Smoking and drinking alcohol reduce the level of male hormones in the blood. To improve hormonal levels, it is recommended:
- sleep at least 7-9 hours at night;
- rest during the day;
- relaxing massage;
- meditation;
- cryosauna;
- regular sexual contacts.

Meditation
How to prevent the formation of the disease
Of course, it is often not possible to find out the cause of the pathology, however, very often it all lies in the fact that the person simply leads an inappropriate lifestyle. It is very important to pay attention to nutrition; you should not consume large quantities of ready-made, semi-finished, canned, or already packaged foods. It is they who often lead to disorders of the hypothalamus very often, this is data from scientific research. The fact is that such food contains chemical substances that cause significant harm to human health, so you need to give them up or certainly seriously reduce them. Excessive alcohol consumption and smoking are of some importance.
Severe damage to the hypothalamus can also develop due to a lack of certain vitamins and microelements in the body, which is also the person’s fault, since a sufficient amount of foods containing such substances necessary for the normal functioning of the human body is not consumed. The hypothalamus has different diseases, but in order to minimize the risk of their occurrence, you don’t need to do anything supernatural - you just need to eat right, follow a daily routine, exercise and get rid of bad habits. It is necessary to prevent head injury; this is often the determining cause of the development of pathology.
CNS tumors and other disorders
Many diseases can lead to menstrual irregularities, including some tumors of the central nervous system, from astrocytomas to gliomas and linealomas. In addition, the causes of such disorders are giant cell arteritis, cavernous sinus thrombosis, tuberculosis, neurofibromatosis (Recklinghausen disease), infiltrative processes such as histiocytosis X (Hand-Schueller-Christian disease). The infundibulum nucleus may be involved in the pathological process. Treatment is medicinal or surgical depending on the nature of the disease.
Diseases that disrupt the anatomy of the central nervous system and cause ovulation disorders
- All tumors
- Giant cell arteritis
- Cavernous sinus thrombosis
- Histiocytosis X
- Tuberculosis
- Syphilis
- Recklinghausen's disease